The Serious Dangers Of Antidepressants Side Effects You NEED To Know Immediately!
Antidepressants side effects and their dangerous long term consequences are hardly ever discussed by physicians when they are prescribed.
According to the latest statistics, 17.3 million American adults (7.1 percent of the adult U.S. population) and 3.2 million adolescents (13.3 percent of U.S. population aged 12 to 17) suffered at least one major depressive episode in 2017.
Depression can interfere with personal and work relationships.
It can also reduce work or academic performance and affect physical health by impairing your ability to properly care for yourself and make good health decisions.
This including decisions about nutrition and sleep. Imbalances in nutrition, weight fluctuations and poor sleep habits may in turn compromise your immune function.
The condition can also be lethal, as depression is a contributing factor in up to 70 percent of all suicides. In 2016, 44,965 Americans committed suicide.
Depression can also lead to self-harming behaviors such as drug or alcohol abuse. And 90 percent of people who struggle with suicidal thoughts experience a combination of depression and substance abuse.
Unfortunately, antidepressant drugs — the most widely used therapy for depression — is also among the least effective.
In fact, statistics suggest that far from being helpful, psychiatric drugs are making the situation worse. Antidepressants side effects being among the main culprits of course.
According to research published in February 2017, 16.7 percent of the 242 million U.S. adults (aged 18 to 85) included in the survey reported filling at least one prescription for a psychiatric drug in 2013.
Twelve percent reported using an antidepressant; 8.3 percent used anxiolytics, sedatives and hypnotics; and 1.6 percent used anti psychotics.
With nearly 17 percent of the adult population in the U.S. taking psychiatric drugs, it would be prudent to evaluate the larger ramifications of these types of medications.
Sadly, statistics overwhelmingly fail to support their use, yet they continue to be the leading form of treatment.
Antidepressants Side Effects: Medication Madness — A Psychiatrist Speaks Out

In a recent segment of Full Measure (above), award-winning investigative journalist Sharyl Atkinson interviewed psychiatrist and director of the International Centre for Patient-Oriented Psychiatry, Dr. Peter Breggin.
He is to many people “the conscience of psychiatry”. He was instrumental in preventing the return of lobotomy as a psychiatric treatment in the early 1970s.

Breggin is also the author of “Medication Madness,” in which he details the many hazards of psychiatric drugs.
In his 50 years of practice, he has never placed a patient on drugs. In fact, he specializes in getting people off them, and wrote a book on psychiatric drug withdrawal. The book is called “Psychiatric Drug Withdrawal: A Guide for Prescribers, Therapists, Patients and Their Families.”
When asked what he thinks people don’t know about psychiatric treatment, and ought to, Breggin responds, “They don’t know that all psychiatric drugs are neurotoxins. Antidepressant side effects don’t even come near their thoughts.
They don’t know that they aren’t correcting biochemical imbalances, they are causing biochemical imbalances.”
Prozac was the first selective serotonin re-uptake inhibitor (SSRI), approved by the U.S. Food and Drug Administration (FDA) in 1987.
Over the years, Prozac was the target of a number of lawsuits, as patients suffered all sorts of ill effects. They ranged from birth defects to suicide and serotonin syndrome.
The latter being a condition caused by excess serotonin in the brain. Moreover it leads to agitation, confusion, high blood pressure and more.
Already by 1996, 35,000 complaints about the drug had been lodged with the FDA.
In the early 1990s, Breggin was appointed by a federal court as the medical and scientific expert for the plaintiffs in all combined lawsuits facing Eli Lilly with regard to Prozac. This role that gave him access to corporate records.
Breggin tells Atkinson:
“Prozac … had amphetamine affects. The chief investigators said and wrote, ‘this drug has amphetamine like effects.
We need to put this into the label. It can make depression worse, can make people agitated, make them angry, might increase the suicide rate’. But the FDA wouldn’t allow onto the label what it’s chief investigator into adverse effects was telling them.
So, from the beginning, it was all a house of cards.
And, as for it’s being useful, I looked it over, carefully analysed the statistics and said the drug actually doesn’t work.
It’s about as good as placebo.
Now, placebo will help anywhere between 40 and 80 percent of people. So it’s a huge effect and that especially with depression, because depression is not about a biochemical imbalance.
It’s about hopelessness. Depression is part of the human experience.”
In Breggin’s view, “There is no promising medical treatment and probably there never can be. For the simple reason that depression is primarily a symptom of altered human emotions and experiences.
He believes one needs to avoid numbing and escapist behaviors such as drug and alcohol use. And implement strategies to support healthy brain function instead, in order to “be able to deal with your issues.”
Contrary to Popular Opinion, Antidepressants Don’t Work
In 2010, an interview with the medical journalist and Pulitzer Prize nominee Robert Whitaker about the use of psychiatric drugs became public domain on the web. He has written two books on this topic.
In it, Whitaker details the science showing antidepressants don’t work — and what actually does.
The available science has also brought Jacob Stegenga, a philosophy of science lecturer at the University of Cambridge and author of “Medical Nihilism,” to the same conclusion. In a recent essay, he notes:
“Diving into the details of how antidepressant data are generated, analysed and reported tells us that these drugs are barely effective, if at all …
The best evidence about the effectiveness of antidepressants comes from randomized trials and meta-analyses of these trials.
The vast majority of these studies are funded and controlled by the manufacturers of antidepressants. This is an obvious conflict of interest.
These trials often last only weeks — far less than the duration that most people are on antidepressants.
The subjects that typically don’t participate to these trials are patients who are elderly. They generally have other diseases, or who are on several other drugs.
In other words, the very kinds of people who are often prescribed antidepressants.
Which mean that extrapolating the evidence from these trials to real patients is unreliable.
The trials that generate evidence seeming to support antidepressants appear on medical journals. While trials that generate evidence suggesting that antidepressants are ineffective often don’t get any attention …
To give one prominent example, in 2012 the U.K. pharmaceutical company Glaxo Smith Kline pleaded guilty to criminal charges for promoting the use of its antidepressant Paxil in children.
There was indeed no evidence that it was effective in children, and for misreporting trial data.
When analysed properly, the best evidence indicates that antidepressants are not clinically beneficial.
Antidepressants Side Effects: What Does the ‘Best Evidence’ Say About Antidepressants?

Some psychiatric drugs may be helpful for a small minority of people with very severe mental health problems, such as schizophrenia.
It’s quite clear that a vast majority of people using these drugs do not suffer from the type of psychiatric illnesses that might warrant their prudent use. They indeed end up worsening their mental health under the hammer of countless antidepressants side effects.
Most are struggling with sadness, grief, anxiety, “the blues” and depression. These are in many ways part of your body’s communication system.
Moreover revealing nutritional or sunlight deficiencies and/or spiritual disconnect, for example.
The underlying reasons for these kinds of troubles are manifold. But you can be sure that, whatever the cause, an antidepressant will not correct it.
In fact, as noted by Breggin…
…studies have repeatedly shown antidepressants work no better than placebo for mild to moderate depression.
Irving Kirsch, associate director of the Program in Placebo Studies at Harvard Medical School, has conducted several meta-analyses of antidepressants side effects in comparison to placebo. He concluded that there’s virtually no difference in their effectiveness.
According to Kirsch, “The difference is so small; it’s not of any clinical importance.”
For example, in a 1998 meta-analysis that looked at 19 double-blind studies, Kirsch and colleagues noted that:
“These data indicate that virtually all of the variation in drug effect size was due to the placebo characteristics of the studies.
The effect size for active medications that we don’t consider to be antidepressants was as large as that for those we generally consider antidepressants.
And in both cases, the inactive placebos gave improvement that was 75 percent of the effect of the active drug.
These data raise the possibility that the apparent drug effect (25 percent of the drug response) is actually an active placebo effect.”
Research published in 2008 found major discrepancies between published and unpublished research. This makes antidepressants appear far more beneficial and effective than the sum total of the research actually reveals them to be.
Of 74 FDA-registered studies, 31 percent were never published.
As noted by the authors, “According to the published literature, it appeared that 94 percent of the completed trials resulted positive.
By contrast, the FDA analysis showed that 51 percent resulted positive …
Selective reporting of clinical trial results may have adverse consequences for researchers, study participants, health care professionals and patients.”
A 2010 meta-analysis concluded that “The magnitude of benefit of antidepressant medication compared with placebo increases with severity of depression symptoms.
And it may be minimal or non-existent, on average, in patients with mild or moderate symptoms.”
In a 2011 paper, Kirsch notes that six-week trials have a higher success rate than eight-week trials. Approx. 55 versus 42 percent. Which suggests long-term use of antidepressants is likely ineffective. And antidepressants side effects are most likely going to take their toll.
In a 2014 paper, Kirsch notes that “analyses of the published data and the unpublished data that were hidden by drug companies reveals that most (if not all) of the benefits are due to the placebo effect.”
In this paper, he notes that two of his earlier meta-analyses actually proved that when both published and unpublished trials were included.
The placebo response accounted for a whopping 82 percent of the beneficial response to antidepressants.
A major benefit of evaluating FDA trial data was that all of the trials used the same primary measure of depression. Which ultimately made the drug-to-placebo effects very easy to identify and compare.
The primary measure of depression used in these studies was the Hamilton depression scale. This is a 17-item scale with a possible score of 0 to 53 points.
The higher your score, the more severe your depression.
Importantly, the mean difference between antidepressants and placebo was less than 2 points (1.8) on this scale.
To illustrate just how insignificant of a difference this is, you can score a 6-point difference. This is achieved simply by changing sleep patterns without any reported change in other depressive symptoms.
Simply fidgeting less results in a 4-point decrease in your depression score, so as noted by Stegenga in his essay…
“a drug that simply made people sleep better and fidget less could lower one’s depression score by 10 points.”
What’s more, clinical guidelines in the U.K. require antidepressants to lower depression scores by a mere 3 points.
And this too reveals why and how the benefits of antidepressants have been overestimated and oversold.
Antidepressants side effects have yet again been sidelined in this instance.
Most recently, a 2017 systematic review with meta-analysis and trial sequential analysis of 131 placebo studies proved that:
“all trials were at high risk of bias and the clinical significance was highly questionable.
SSRIs significantly increase the risk of both serious and non-serious adverse events.
The potential small beneficial effects seem to be outweighed by harmful effects.”
None of the trials, even when reporting a positive result, met the threshold for clinical significance of 3 points on the depression score.
Antidepressants Side Effects: Long-Term, Antidepressant Users Fare Much Worse
 What’s more, research has shown that patients who do not take antidepressants fare better in the long term compared to those taking drugs, and research comparing exercise and drug treatment for depression suggests those not taking drugs have a lower risk of relapse.
What’s more, research has shown that patients who do not take antidepressants fare better in the long term compared to those taking drugs, and research comparing exercise and drug treatment for depression suggests those not taking drugs have a lower risk of relapse.
This risk is also addressed in Kirsch’s 2014 paper on antidepressants and the placebo effect.
“The serotonin theory is as close as any theory in the history of science to having been proved wrong.
Instead of curing depression, popular antidepressants may induce a biological vulnerability. Thus making people more likely to become depressed in the future,” Kirsch writes.
This is further evidence that antidepressants side effects overwhelmingly outweigh the very little benefits they claim to bring in.
Known Side Effects Of Antidepressants
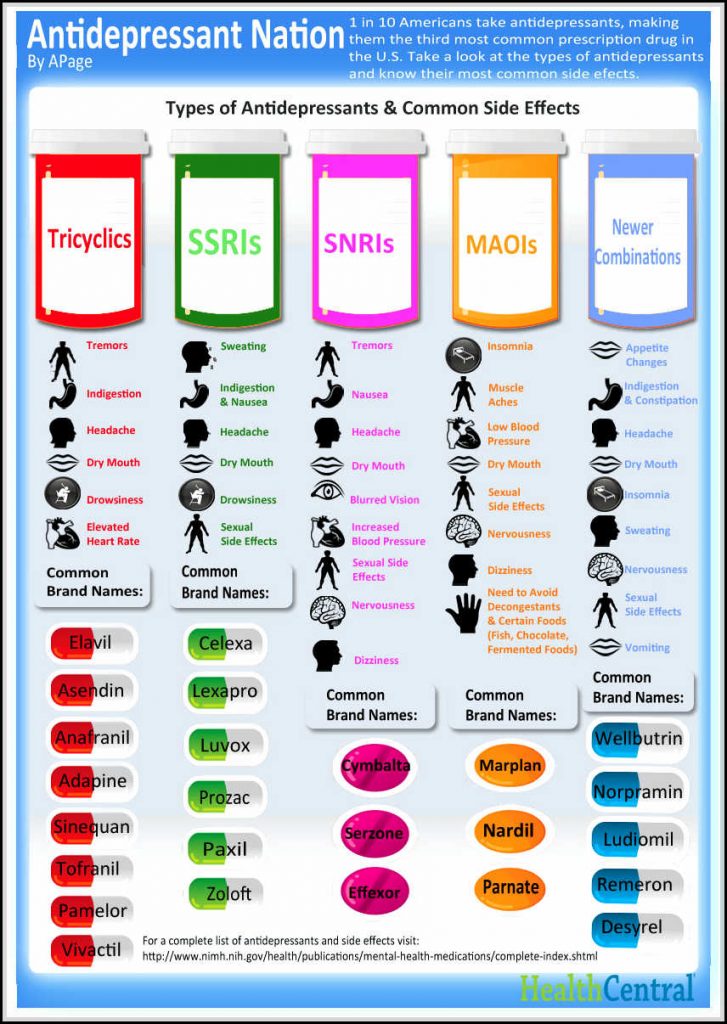
In addition to not working better than placebo, antidepressants also have a long list of potential side effects. These include but are not limited to:
| Worsening depression |
| Self-harm, violence and suicide |
| Increased risk of developing Type 2 diabetes,33 even after adjusting for risk factors such as body mass index34 |
| Thickening of the greater carotid intima-media (the lining of the main arteries in your neck that feed blood to your brain), which could contribute to the risk of heart disease and stroke. This was true both for SSRIs and antidepressants that affect other brain chemicals |
| An increased risk of heart attack, specifically for users of tricyclic antidepressants, who have a 36 percent increased risk of heart attack |
| An increased risk of dementia; as the dose increases, so does the risk for dementia |
| Depletion of various nutrients, including coenzyme Q10 and vitamin B12 — in the case of tricyclic antidepressants — which are needed for proper mitochondrial function. SSRIs have been linked to iodine and folate depletion |
Depression Treatments That Actually Work

If you’re at all interested in following science-based recommendations, you’d place antidepressants at the very bottom of your list of treatment candidates.
Far more effective treatments for depression include:
ExerciseA number of studies have shown exercise outperforms drug treatment. Exercise helps create new GABA-producing neurons that help induce a natural state of calm. Likewise it boosts serotonin, dopamine and norepinephrine, which helps buffer the effects of stress. Studies have shown there is a strong correlation between improved mood and aerobic capacity. But even gentle forms of exercise can be effective. Yogafor example, has received particular attention in a number of studies. One study found 90-minute yoga sessions three times a week reduced symptoms of major depression by at least 50 percent. |
Nutritional interventionKeeping inflammation in check is an important part of any effective treatment plan. If you’re gluten sensitive, you will need to remove all gluten from your diet. Reducing lectins also be a good idea. As a general guideline, eating a whole food diet as described in my optimal nutrition plan can go a long way toward lowering your inflammation level. A cornerstone of a healthy diet is limiting sugar of all kinds. Ideally to no more than 25 grams a day. In one study, men consuming more than 67 grams of sugar per day were 23 percent more likely to develop anxiety or depression. This is over the course of five years than those whose sugar consumption was less than 40 grams per day. Certain nutritional deficiencies are also notorious contributors to depression, especially:
|
Vitamin DStudies have shown vitamin D deficiency can predispose you to depression. And that depression can respond favorably to optimizing your vitamin D stores, ideally by getting sensible sun exposure. In one study, people with a vitamin D level below 20 nanograms per millilitre (ng/mL) had an 85 percent increased risk of depression. This is compared to those with a level greater than 30 ng/mL. A double-blind randomized trial published in 2008 concluded that supplementing with high doses of vitamin D seems to ameliorate depression symptoms. Thus indicating a possible causal relationship. “Recent research also claims that low vitamin D levels appear to be associated with suicide attempts. For optimal health, make sure your vitamin D level is between 60 and 80 ng/mL year-round. Ideally, get a vitamin D test at least twice a year to monitor your level. |
Light therapyLight therapy alone and placebo were both more effective than Prozac for the treatment of moderate to severe depression in an eight-week long study. Spending time outdoors in broad daylight is the least expensive and likely most effective option. |
ProbioticsKeeping your gut micro biome healthy also has a significant effect on your moods, emotions and brain. You can read more in my previous article, “Mental Health May Depend on the Health of Your Gut Flora.” |
Emotional Freedom Techniques (EFT)EFT is a form of psychological acupressure that proved to be quite effective for depression and anxiety. For serious or complex issues, seek out a qualified health care professional who is trained in EFT to guide you through the process. That said, for most of you with depression symptoms, this is a technique you can learn to do effectively on your own. |
Other Helpful Treatment Strategies
Here are several additional strategies that can help improve your mental health:
Minimize electromagnetic field (EMF) exposureIn 2016, Martin Pall, Ph.D., published a review in the Journal of Neuro anatomy showing how microwave radiation from cellphones, Wi-Fi routers and computers and tablets not in airplane mode is clearly associated with many neuro-psychiatric disorders. These electromagnetic fields (EMFs) increase intracellular calcium. And therefore they trigger the production of extremely damaging free radicals by acting on your voltage gated calcium channels (VGCCs). And the tissue with the highest density of VGCCs is your brain. Once these VGCCs are stimulated they also cause the release of neurotransmitters and neuro-endocrine hormones. These hormones contribute not only to anxiety and depression but also neuro-degenerative diseases like Alzheimer’s. So, if you struggle with anxiety or depression, be sure to limit your exposure to wireless technology. Simple measures include turning your Wi-Fi off at night, not carrying your cellphone on your body unless it’s in airplane mode. And also not keeping portable phones, cellphones and other electric devices in your bedroom. |
Clean up your sleep hygieneMake sure you’re getting enough high quality sleep, as sleep is essential for optimal mood and mental health. The inability to fall asleep and stay asleep can be due to elevated cortisol levels, so if you have trouble sleeping, you may want to get your saliva cortisol level tested with an Adrenal Stress Index test. Adaptogens, herbal products that help lower cortisol and adjust your body to stress, can be helpful if your cortisol is running high. There are also other excellent herbs and amino acids that help you to fall asleep and stay asleep. For more tips and guidelines, see “Sleep — Why You Need It and 50 Ways to Improve It” from Dr Mercola. |
Optimize your gut healthA number of studies have confirmed gastrointestinal inflammation can play a critical role in the development of depression. Optimizing your gut micro biome will also help regulate a number of neurotransmitters and mood-related hormones, including GABA and corticosterone, resulting in reduced anxiety and depression-related behaviour. To nourish your gut micro biome, be sure to eat plenty of fresh vegetables and traditionally fermented foods such as fermented vegetables, lassi, kefir and natto. If you do not eat fermented foods on a regular basis, taking a high-quality probiotic supplement is recommended. Also remember to severely limit sugars and grains, to re-balance your gut flora. |
VisualizationVisualization and guided imagery have been used for decades by elite athletes before an event, successful business people and cancer patients — all to achieve better results through convincing your mind you have already achieved successful results. Similar success has been found in people with depression. |
Cognitive behavioral therapy (CBT)CBT has been used successfully to treat depression. This therapy assumes mood is related to the pattern of thought. CBT attempts to change mood and reverse depression by directing your thought patterns. |
Make sure your cholesterol levels aren’t too low for optimal mental healthYou may also want to check your cholesterol to make sure it’s not too low. Low cholesterol is linked to dramatically increased rates of suicide, as well as aggression toward others. This increased expression of violence toward self and others may be due to the fact that low membrane cholesterol decreases the number of serotonin receptors in the brain. And they are approximately 30 percent cholesterol by weight. Lower serum cholesterol concentrations therefore may contribute to decreasing brain serotonin. This not only contributes to suicidal-associated depression, but prevents the suppression of aggressive behaviour and violence toward self and others. |
Eco therapyStudies have confirmed the therapeutic effects of spending time in nature. Eco therapy lowers stress, improves mood and significantly reduces symptoms of depression. Outdoor activities could be just about anything, from walking a nature trail to gardening, or simply taking your exercise outdoors. |
Breathing exercisesBreath work such as the Buteyko breathing technique also has enormous psychological benefits and can quickly reduce anxiety by increasing the partial pressure of carbon dioxide in your body. |
Helpful supplementsA number of herbs and supplements can be used in lieu of drugs to reduce symptoms of anxiety and depression. These include:
|
Antidepressants Side Effects: Guidelines for Safe Drug Withdrawal

If you’re currently on an antidepressant and want to get off it, ideally, you’ll want to have the cooperation of your prescribing physician.
It would also be wise to do some homework on how to best proceed.
Breggin’s book, “Psychiatric Drug Withdrawal: A Guide for Prescribers, Therapists, Patients and Their Families,” and/or “The Antidepressant Solution: A Step-by-Step Guide to Overcoming Antidepressant Withdrawal, Dependence, and Addiction” by Dr. Joseph Glenmullen can be helpful.
You can also turn to an organization with a referral list of doctors who practice more biologically or naturally, such as the American College for Advancement in Medicine at www.acam.org.
A holistic psychiatrist will have a number of treatment options in their tool box that conventional doctors do not. And he will typically be familiar with nutritional supplementation.
Once you have the cooperation of your prescribing physician, start lowering the dosage of the medication you’re taking.
There are protocols for gradually reducing the dose that your doctor should be well aware of.
 At the same time, it may be wise to add in a multivitamin and/or other nutritional supplements or herbs.
At the same time, it may be wise to add in a multivitamin and/or other nutritional supplements or herbs.
Again, your best bet would be to work with a holistic psychiatrist who knows his way around the use of nutritional support.
If you have a friend or family member who struggles with depression, perhaps one of the most helpful things you can do is to help guide them toward healthier eating and lifestyle habits.
Moreover making changes can be particularly difficult when you’re feeling blue or worse, suicidal.
Encourage them to unplug and meet you outside for walks.
We should not underestimate the power of human connection, and the power of connection with nature.
Both, I believe, are essential for mental health and emotional stability.
Did you know? The American Psychological Association (APA) reported in 2015 that 72% of adults feel stressed.
 Most respondents cited work and money as the causes of stress.
Most respondents cited work and money as the causes of stress.
In addition to healthy lifestyle practices, a plethora of research indicates that, unlike antidepressants, certain nutrients can help sustain and promote excellent brain function as we age.
If you’re concerned about maintaining healthy brain function well into your 70s, 80s and beyond, (and who isn’t?), you’ve got to make sure you’re getting enough of the nutrients your brain craves to maintain sharp memory.
We are highly selective in our choice of brain supplements for two reasons:
(1) this is a highly saturated market that one needs to set real winners apart from less optimally performing products, and
(2) brain potency and wellness benefits are quite easy to claim and therefore one has to be discriminating in choosing.
Having said that, following years of trials and errors the speed and precision at which this so called transfer factor formula responds to brain enhancement needs is truly impressive.
And without unwanted effects that could turn off first-time users.
The benefits are sustained and evident from first dose, and this doesn’t happen every time with nootropic products.
This unique formula is one worth exploring for its premium quality and value for money.
This is an impressive proprietary blend that helps lower anxiety and susceptibility to stress
It’s tailored for busy individuals who wish to improve their overall mood, cognitive focus, and ability to cope with stress in daily life
Among the key benefits are:
- Daily support for a positive mood
- Enhances your ability to cope with the daily stresses of life
- Promotes relaxation, a positive mood, and the ability to focus
- Supports the immune system’s ability to function properly in times of occasional stress
The proprietary blend of extensively researched natural ingredients. These include L-Theanine and Wild Green Oat (Avena sativa), supports brain and circulatory system function.
Also it promotes healthy physiological responses to occasional stress, including blood pressure and heart rate
But on top of my list are these top key features that quite frankly I wouldn’t trade for anything else:
- Contains transfer factors (immune messenger molecules) that help educate immune cells and promote the immune system’s ability to more effectively recognize, respond to, and remember threats
- Alleviates some of the temporary negative physiological responses that accompany occasional mental stress—including changes in heart rate, blood pressure, and immune system response
Check This Out – Europe Only
Check This Out – Rest Of The World
Keep on working, great job!
Fairly certain he will have a good read. Thank you for sharing!